March 2021
Paeudotrichoscopic findings from colour product use: a retrospective analysis & a test to reproduce findings
M. Sachdeva, M. Kinoshita-Ise and N.H. Shear
This article describes in a unique retrospective study in a systematic approach the artificial trichiscopoc findings produced as a result of cosmetic hair colour products applied to the scalp that can misguide the diagnosis.
Methodology & Findings
The study was approved by the ethics committee at sunny brook Health Science Centre.
The authors reviewed trichiscopic images of 193 patients and healthy volunteers visiting their hair clinic between 09/8/2018–09/8/2019. They identified 21 cases ( 20 females and 1 male) with artificial findings. Of these cases 15 had (71.4%) had female pattern hair loss / androgenic alopecia (FPHL/AGA), 2(9.5%) had lichen planopilaris, 2(9.5%) had no hair disease, 1 (4.8%) had traction alopecia, and 1(4.8%) had Alopecia Areata.
Five patients (23.8%) used fibre hair products and four patients (19.1%) used liquid products according to the medical records.The types of hair products used by the remaining 12 patients (57.1%) were not reported.
The various ‘mimicry’
The pseudo trichoscopy findings mimicked black dots in 14 cases (66.7%) broken hair in 10 cases (47.6%) and peripilar signs in two cases. Apart from this the dye demonstrated irregular interfollicular pigmentation in six cases (28.6%) and irregular perifollicular pigmentation in five
(23.8%), which did not resemble any well-recognised trichiscopic findings. With fibre-type products, broken hairs were the most frequent (100%,n=5), followed by short vellus hairs (49%,n=2). Of note thick fibres resembled broken hairs whereas thin fibres mimicked short vellus hairs. With liquid hair products black dots were the most frequent pseudo trichoscopy findings (75%,n=3). Hair diameter diversity was the most frequent real finding (71.4%)
The lemon peel experiment
The authors subsequently experimented to reproduce the similar trichiscopic findings on lemon peel by applying different types of hair dyes. Scattered artefacts from fibre hair products mimicked broken and short vellus hairs while those of liquid products were visible over the interdent spaces resembling black dots, or around the. dents resembling , peripilar sign. Powder hair products were diffusely distributed and developed as irregular stains.
Conclusion
The authors demonstrated and highlighted the association between the types of hair colour products and their pattern of distribution and staining. Fibre dyes were strongly associated with broken hairs and sometimes with short vellus hairs, while liquid and powder types were more likely to result in irregular staining. Given that the majority of patients had FPHL/AGA, the increased number of hair ostias without terminal hairs might have allowed the due to penetrate the follicles easily and produce follicular signs. However, as the hair dyes also stained intrafollicular spaces, caution should be noted regardless of the underlying disease. Careful history-taking and enquiry about hair products before and during the medical examination would be useful to exclude pseudo trichoscopic signs.
Drug-induced Alopecia Areata?
A.Murad, J.Maguire and W.Bergfeld.
The authors report a case of Drug Induced Alopecia Areata (DIAA) associated with Lansoprazole followed by a literature review.
Case report
A healthy white woman in her 40s presented with a 4-day history of generalised urticaria eruption and scalp pruritis which occurred 4 days after she was started on lansoprazole for gastritis.She had no joint pain or fever.She was not on other medications and had no history of allergy to any medication. Three weeks into the lansoprazole treatment she noticed a patch of Alopecia on her scalp, which rapidly evolved into a diffuse thinning of the scalp.Lansoprazole was replaced with ranitidine and she was commenced on prednisolone 40mg tapered over 6 weeks to treat the rash and alopecia. Although the rash improved the Alopecia progressed rapidly to alopecia totalis.
All kab investigations including autoimmune profile were normal or negative.
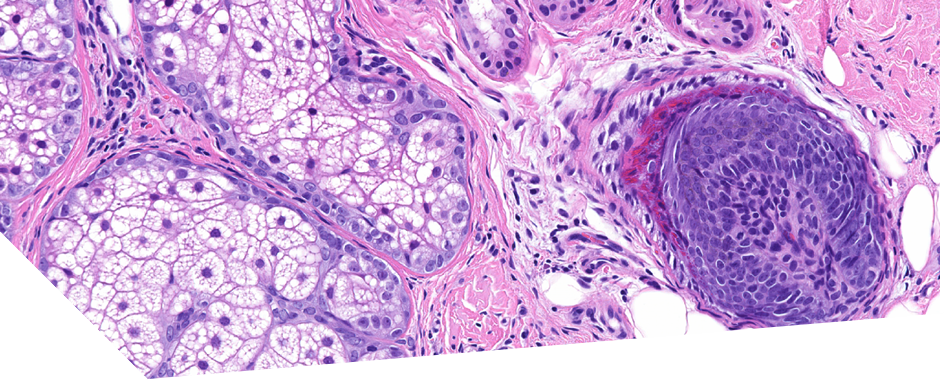
Histopathology of a scalp biopsy revealed peribulbar lymphohistiocytic infiltrate with the classical ‘swarm of bees’ appearance and melanophages surrounding the bulb of the hair follicle. The patient was treated with topical clobetasol propionate 0.05% lotion once daily to her scalp and the regrowth of hypopigmented hair was noted after 4 weeks of treatment. Eight weeks later treatment was tapered to application once or twice weekly until it was stopped after 12 weeks.There was complete hair regrowth after 16 weeks which remained uniformly hypopigmented at the 2 year follow up.
The presence of the eruption that preceded the alopecia , the rate of recovery and the sustained remission of the alopecia despite minimal treatment after discontinuation of the medication are supportive and in favour of DIAA. A differential diagnosis would be drug hypersensitivity reaction that occurred concurrently with AA. In the absence of a specific assay to confirm the drilling induced aetiology it is difficult to discriminate between these possibilities.
Summary of Literature Review
DIAA is a relatively understudied subtype of AA. A review of the literature done by the authors revealed that it shares similar demographic features and disease outcome with IAA. The mean age of reported patients was 42.5 years
and the mean insect following medication was 3.8 months. The majority of reported cases involved monoclonal antibodies (73.7%). Five patients (36%) had patchy regrowth, four (29%) had complete regrowth and three (21%) had regrowth with poliosis and three (21%) did not experience any regrowth.
The authors have tabulated all the reported cases of drug-induced alopecia areata between 2001 -2019. The table lists the age and sex of the patient, medication involved, time taken for onset of symptoms, type of alioecia and treatment outcome ( as summarized above).
Below is the summarised list of the offending drug and time of onset per study-
Rifampicin (2 weeks, 6 weeks)
Phenobarbitone (2 months)
Adalimumab (12 months)
Acitretin (1month)
Abacavir (3 month)
Denosumab (2 weeks)
Sulphasalazine (9 months)
Anti-PDL-1 (6,3,15 months)
Alemtuzumab (4.5,6 months)
Carbocysteine (7days)
Nivolumab( 2,4,6,15 months)
Dupilumab (1.5,2,4,26 months)
Secukinumab (6 months)
Conclusion
The authors understand that it’s difficult to confirm direct causality between the medication and Alopecia in their reported case. Although reintroduction of the offending agent to reproduce the alopecia would have helped confirm the diagnosis further however owing to ethical and safety reasons this was not deemed appropriate in case of their patient. But stopping the lansoprazole did result in complete resolution of the rash and the alopecia.The sustained regrowth of hypopigmented hair supports the hypothesis that pigment art mechanisms are primary targets in the pathogenesis of of AA.
The striking picture of Snow White hair on the back of the head can be seen on the front cover of the March 2021 edition of the CED.
As with most drug induced dermatosis a detailed drug history should always be established with timely cessation of the implicated medication to ensure good patient outcome.
Homozygous dominant missense mutation in Keratin 6b leading to severe pachyonychia congenita (PC)
J Mathews, C.D Hansen, L.Chandrasekhar
In this CPD article the authors discuss a case report of a rare homozygous manifestation of PC; a missense mutation in KRT6B gene, which showed a more aggressive phenotype than usually seen in this group , more similar to that seen in KRT6A mutation.
Case report
A 3 year old girl presented with severe plantar pain , palmo plantar callosities and thickened nails. The child was not able to walk more than a few meters at a time due to the severity of the plantar pain. There was no history of natal teeth , breathing or feeding difficulties in infancy. The parents were consanguineous. Pedigree analysis revealed an autosomal dominant pattern of inheritance. None of the family members had sought treatment as callosities were common in family and were not associated with any functional limitation.
Physical examination showed focal keratoderma over the soles, focal palmar callosities including
including lesions on the interphalangeal creases
(the later feature is unusual in PC). All 20 nails were dystrophic with massive subungual hyperkeratosis. Follicle based hyperkeratotic spiny papules were present over the dorsal hands and the elbows, axilla , buttocks, knees and ankles. There was no oral leukokeratosis or hyperhidrosis.
Both parents had focal keratoderma of soles requiring frequent pairing , but plantar pain was minimal. Focal callosities were present on the palms. All 10 toenails were dystrophic in the father whereas only the great toes were affected in the mother. The parents did not have any fingernail dystrophy or follicular applies. The child had a 18 month old sister who was apparently normal.
Genetic analysis
Following informed consent from parents a homozygous missense mutation in the KRT6B gene, NM_005555.3:c.1414G>A (p.Glu472Lys) was identified in the child using a nine gene panel designed using Agilent SureSelect ( me genomics , Alpharetta, GA, USA) to include KRT6A, KRT6B, KRT6C, KRT16, KRT17, DSG1, TRPV3 , GJB6 and AAGAB genes. The variant was confirmed by Sanger sequencing. Both parents and the younger sister were heterozygous for the same mutation.
The mutation has been previously reported in 53 individuals from 19 families with PC, though not in a homozygous form.
Conclusion.
The only other report of a homozygous mutation in keratopathy reported was one from PC. Wilson et al, who reported 2 families with missense mutation in KRT17 in whom homozygosity resulted in a more severe disease compared with heterozygous individuals, with alopecia as an additional feature.
In general the mutations in PC can be classified as having severe phenotype in KRT6A, intermediate in KRT6B and mild in KRTC
The authors have reported this unique case to highlight the fact that homozygous mutation in KRT6B can produce a more severe phenotype similar to KRT6A.
Homozygosity must be considered when an individual is more severely affected than other family members, particularly in families with vivo known consanguinity. Genetic counselling is important in these families.
Investigating human eyelash hair follicle growth in situ and ex civil: a pilot study
C.I. Platt, J Laybourne, P. Cannon, R. Paus
This study shows for the first time that organ culture of human ELHF (eyelash hair follicles) is possible in principle, where the clinically crucial switch from anagen to catagen, and eyelash production as such can be studied and pharmacologically manipulated ex vivo.
For this study eyelid biopsies were collected from three patients ( mean number of ELHFs examined per biopsy 14+/-3) undergoing lower- lid correction at the Manchester Royal Eye Hospital. All ELHFs within a biopsy were microdissected, snap frozen and cryosectioned at 7 micrometer.ELHFs in the anagen, early anagen, telogen and catagen stages were identified.
Ex vivo the ELFHs were observed and studied for change in growth pattern and variability in pigmentation and the findings were documented.
This study extends previous human ELHF work by examining not only anagen but also telogen, catagen and early anagen ELHF and by showing that these stages are similar to those in human scalp HFs (hair follicles)
Although limited by the low number of organ -cultured anagen ELHFs that could be examined this pilot study demonstrates that theEKHFs can be microdissected and organ cultured, thus substantially expanding the methodological repertoire of human eyelash research.
A qualitative exploration of the experiences of the adolescents with Alopecia areata and their messages for healthcare professionals.
I de Vere Hunt, A. McNiven and T. McPherson
In this secondary inductive thematic analysis of 21 in depth semi structured interviews with young people with Alopecia Areata( AA) the authors have demonstrated the psychological impact of this disease in the adolescent subjects.
The age range of the participants were 14-23, eighteen females and three males.The core emotional and psychological themes identified by the analysis are (1). Isolation and Community: most participants identified alopecia as “a hidden problem” and “felt very alone” when diagnosed. However, many found tremendous support in online forums and support groups in which they could share experiences with other people with AA. (2). Self- consciousness: participants cited feeling “paranoid” at being stared at, sometimes to the extent that they could not leave the house.(3).”It’s not just hair”: the concept of AA being far more than hair loss was prominent throughout; some felt they lost their identity and some young woman felt it had impacted there “femininity”. Societal connotations of hair loss also frequently posed a challenge with many people presuming that young people with AA had cancer.(4). Unpredictability: some participants described “not knowing “ whether their hair would grow back as the most difficult part of their experience, and were ”living in fear” that their hair would fall out again even after experiencing regrowth.Some individuals recounted shaving off their hair as a way of taking back control in their tumultuous disease course.
There was a notable heterogeneity among the participant responses.Although the majority felt that their Alopecia had been tremendously difficult, others felt that it had made them a better and/or a unique person.A conflict in perspectives was sometimes observed within individual participant accounts, likely reflecting both the ongoing ‘alopecia journey’ and adolescence as a time of major change.
An awareness of these complex psychological themes is crucial to provision of high-quality, developmentally appropriate care for adolescents with AA.Via analysis of the whole transcripts the authors identified two overarching messages for healthcare professionals managing adolescents with AA ; (1) give more information and (2)address the emotional impact (see the original article in BJD March 2021 edition for illustrative data extracts)
One of the participants recounted that “ they didn’t give me any information on wigs or anything which was quite tough, because we didn’t realise that I was entitled to free wigs”.
Although the British Association of Dermatologists guidelines for the management of AA recommend considering psychological support, the participants in the interview frequently cited a failure of their general practitioners or dermatologist to do so. This echoed in existing literature ; in a questionnaire-based study investigating the effect of alopecia on quality of life, 40% of the respondents reported feeling that their doctors had been either ‘insensitive’, ‘dismissive’ or ‘unsupportive’.
There are likely several reasons for the failure of many healthcare professionals to address the emotional impact of AA, including consultation time constraints, but it is essential.
For many young people Alopecia is their first experience of navigating health services and adjustment to a chronic condition may be overwhelming , while also dealing with the conspicuous nature of Alopecia during a critical time in development of self.
The authors suggest that increased awareness of the emotional issues patients might be experiencing, combined with an appreciation of the valuable role of the appropriate online support and information, will better equip healthcare professionals